Baby Acne Treatment: Safe and Effective Ways to Clear Infant Acne Fast
Discover the best Baby Acne Treatment methods, including safe home remedies, causes, symptoms, prevention tips, and expert advice for clearing infant acne fast.
Explore a complete 2026 guide to tms therapy, including benefits, side effects, procedure, and how it treats depression effectively in modern psychiatry
In recent years, mental health treatment has evolved rapidly, and one of the most promising breakthroughs is tms therapy. As depression rates continue to rise globally in 2026, researchers and clinicians are turning to innovative, non-invasive treatments that offer hope to patients who do not respond well to traditional medication.
tms therapy (Transcranial Magnetic Stimulation) has become a widely discussed option in psychiatry due to its ability to stimulate specific areas of the brain associated with mood regulation. Unlike medications, it does not involve systemic chemicals, making it an appealing alternative for many patients.
In this in-depth guide, we will explore what tms therapy is, how it works, its benefits, side effects, effectiveness in treating depression, and why it is becoming a key part of modern mental health care in 2026.
Table of contents [Show]
tms therapy stands for Transcranial Magnetic Stimulation, a non-invasive medical procedure that uses magnetic fields to stimulate nerve cells in the brain.
The treatment primarily targets the prefrontal cortex, a region responsible for mood control and emotional regulation. In individuals with depression, this area is often underactive. tms therapy helps “reactivate” these brain circuits, improving mood and reducing depressive symptoms.
Unlike electroconvulsive therapy (ECT), tms therapy does not require anesthesia and does not cause memory loss, making it a safer and more tolerable option for many patients.
To understand the effectiveness of tms therapy, it is important to look at its mechanism of action.
During a tms therapy session:
By repeatedly stimulating these brain regions, tms therapy helps improve communication between neurons, which is often disrupted in depression.
One of the primary uses of tms therapy is the treatment of major depressive disorder (MDD), especially in patients who have not responded to antidepressant medications.
Clinical studies show that tms therapy can significantly reduce depressive symptoms in many patients. Some even achieve full remission after a complete treatment cycle.
In 2026, tms therapy is widely recognized as an evidence-based treatment for:
There are several reasons why tms therapy has become increasingly popular in mental health care.
Unlike surgical or invasive brain procedures, tms therapy does not require incisions or anesthesia.
Because tms therapy does not involve medication, it avoids many common drug-related side effects such as weight gain or fatigue.
Patients undergoing tms therapy can return to their normal daily activities immediately after each session.
Unlike electroconvulsive therapy, tms therapy does not affect memory or cognitive function.
For individuals who do not respond to antidepressants, tms therapy provides a new path to recovery.
tms therapy is typically recommended for:
However, not everyone is a suitable candidate. A psychiatric evaluation is required before starting tms therapy.
A typical tms therapy treatment follows a structured process:
A psychiatrist evaluates the patient’s mental health history.
The technician identifies the exact area for stimulation.
Each tms therapy session lasts about 20–40 minutes.
Patients usually undergo tms therapy 5 days a week for 4–6 weeks.
Doctors track improvements in mood and behavior.
Although tms therapy is considered safe, some side effects may occur:
These effects are usually temporary and subside shortly after treatment.
Serious side effects from tms therapy are extremely rare, making it one of the safest brain stimulation treatments available.
Recent advancements have significantly improved the success rate of tms therapy.
Studies show that:
In 2026, optimized protocols and AI-guided targeting have made tms therapy even more precise and effective.
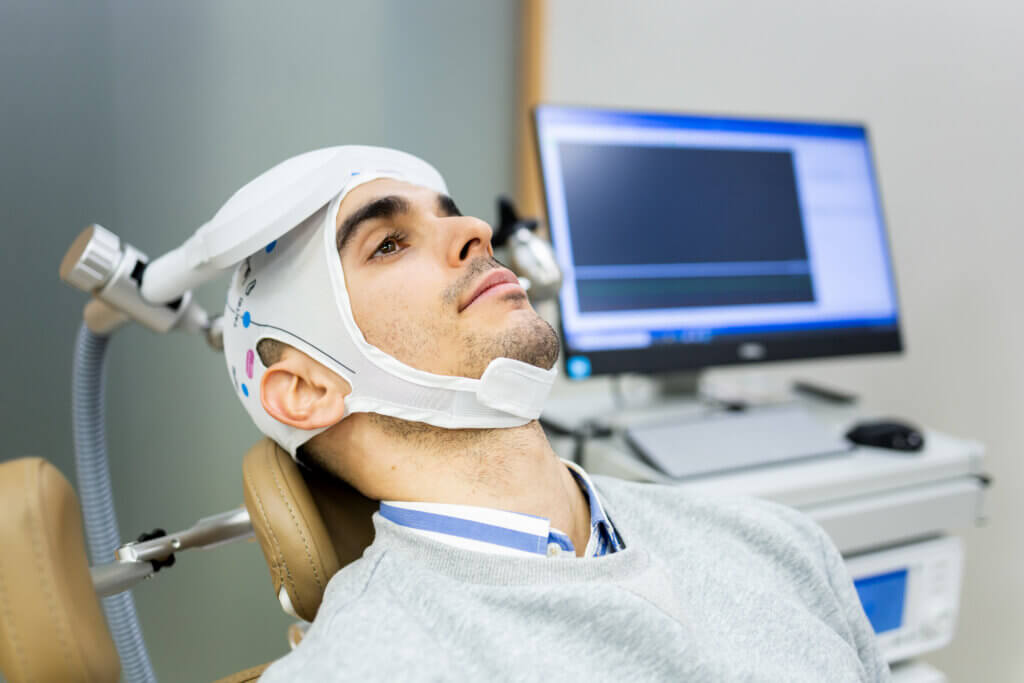
When comparing treatment options, tms therapy offers several advantages over traditional antidepressants:
For many patients, tms therapy becomes a preferred alternative when medications fail.
Modern neuroscience supports the effectiveness of tms therapy. Research shows that repetitive magnetic stimulation can:
In 2026, ongoing studies continue to refine tms therapy, making it more personalized and effective.
Despite its benefits, tms therapy does have some limitations:
Understanding these limitations helps set realistic expectations for tms therapy outcomes.
Today, tms therapy is considered a major advancement in psychiatric treatment. Many mental health clinics now include it as part of comprehensive depression care programs.
Its integration into mainstream medicine highlights how far brain stimulation therapies have come.
The future of tms therapy looks promising, with several innovations emerging:
Artificial intelligence is helping improve the precision of tms therapy targeting.
Researchers are developing smaller devices for home-based tms therapy.
Future tms therapy sessions may be tailored to each patient’s brain activity patterns.
Beyond depression, tms therapy may be used for PTSD, anxiety, and addiction.
There are several misconceptions about tms therapy:
In reality, tms therapy causes only mild discomfort.
tms therapy is FDA-approved and widely used in clinical practice.
tms therapy does not alter personality or identity.
Many patients report life-changing improvements after tms therapy. Individuals who struggled with long-term depression often describe renewed energy, better sleep, and improved emotional stability.
These outcomes demonstrate the growing importance of tms therapy in mental health recovery.
Yes, tms therapy is considered very safe with minimal side effects.
Most patients notice improvements within 2–4 weeks of tms therapy.
In many countries, insurance may partially or fully cover tms therapy for depression.
In 2026, tms therapy stands as one of the most innovative and effective treatments for depression, especially for those who have not found relief through medication. Its non-invasive nature, strong scientific backing, and growing success rates make it a powerful tool in modern psychiatry.
While not a universal solution, tms therapy offers hope, especially for treatment-resistant depression. As technology advances, its role in mental health care is expected to expand even further.
Ultimately, tms therapy represents a shift toward safer, more targeted, and more effective brain-based treatments—reshaping the future of mental health care worldwide
Discover the best Baby Acne Treatment methods, including safe home remedies, causes, symptoms, prevention tips, and expert advice for clearing infant acne fast.
Learn everything about Facet Arthropathy, including symptoms, causes, diagnosis, and the best treatment options for managing spinal joint pain and improving mobility
Learn everything about Mastoid Effusion, including causes, symptoms, diagnosis, treatment options, complications, and prevention tips for better ear health
These cookies are essential for the website to function properly.
These cookies help us understand how visitors interact with the website.
These cookies are used to deliver personalized advertisements.

