Corn vs Wart Explained: Causes, Treatment, and Easy Identification Tips
Learn the complete Corn vs Wart comparison, including causes, symptoms, treatment options, prevention strategies, and easy ways to identify the difference quickly
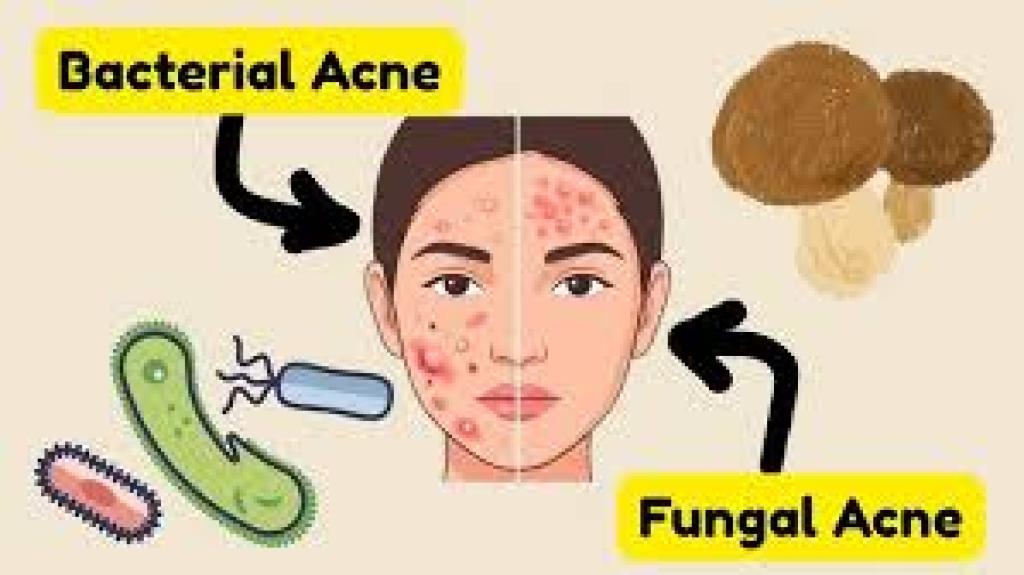
Learn the key differences between fungal vs bacterial acne, including symptoms, causes, treatment options, and expert skincare tips for clear skin in 2026.
Acne is one of the most common skin conditions worldwide, affecting millions of people across all age groups. However, not all acne is the same. Two of the most commonly confused types are fungal acne and bacterial acne.
Understanding the difference between them is essential because using the wrong treatment can actually make the condition worse. This is why learning about Fungal vs Bacterial Acne is so important for proper skin care and long-term skin health.
In this complete 2026 guide, we will break down everything you need to know about Fungal vs Bacterial Acne, including causes, symptoms, diagnosis, treatment options, and prevention strategies.
Table of contents [Show]
Despite its name, fungal acne is not true acne. It is a skin condition caused by yeast overgrowth in hair follicles.
The medical term is:
Malassezia Folliculitis
It happens when a type of yeast called Malassezia grows uncontrollably on the skin, leading to inflammation and breakouts.
Many people mistakenly treat fungal acne like regular acne, which is why understanding Fungal vs Bacterial Acne is critical.
Bacterial acne is the classic form of acne that most people are familiar with.
It is medically associated with:
Acne Vulgaris
This type of acne is caused by:
When comparing Fungal vs Bacterial Acne, bacterial acne is far more common and well-studied.
Understanding Fungal vs Bacterial Acne starts with identifying their core differences.
These differences are key in identifying Fungal vs Bacterial Acne correctly.
Common signs include:
When evaluating Fungal vs Bacterial Acne, itchiness is a major clue.
Typical symptoms include:
Unlike fungal acne, bacterial acne is usually not itchy.
Fungal acne develops due to an imbalance in skin flora.
Common triggers include:
Understanding these causes helps differentiate Fungal vs Bacterial Acne more clearly.
Bacterial acne develops when pores become clogged.
Main causes include:
Proper diagnosis is essential in treating Fungal vs Bacterial Acne effectively.
Fungal acne requires antifungal treatment, not antibiotics.
Using antibiotics can worsen fungal acne, which is why understanding Fungal vs Bacterial Acne matters.
Bacterial acne treatments focus on reducing bacteria and oil production.
A fungal acne-safe routine includes:
Avoid heavy oils and fermented ingredients.
For bacterial acne:
Many people misdiagnose their acne, leading to incorrect treatment.
Avoiding these mistakes is key in understanding Fungal vs Bacterial Acne.
Diet plays a role in both types of acne.
Lifestyle also impacts Fungal vs Bacterial Acne:
To prevent fungal acne:
To prevent bacterial acne:
They are different conditions, but misdiagnosis or improper treatment can cause overlapping symptoms. Understanding Fungal vs Bacterial Acne prevents confusion.
Seek medical help if:
When comparing Fungal vs Bacterial Acne, remember:
Correct diagnosis leads to faster and more effective treatment.
Understanding Fungal vs Bacterial Acne is essential for anyone struggling with persistent skin issues. Although they may look similar at first glance, they are completely different conditions requiring different treatments.
With proper identification, skincare routine, and sometimes medical guidance, both conditions can be effectively managed and controlled
Learn the complete Corn vs Wart comparison, including causes, symptoms, treatment options, prevention strategies, and easy ways to identify the difference quickly
Discover the best Baby Acne Treatment methods, including safe home remedies, causes, symptoms, prevention tips, and expert advice for clearing infant acne fast.
Learn everything about Facet Arthropathy, including symptoms, causes, diagnosis, and the best treatment options for managing spinal joint pain and improving mobility
These cookies are essential for the website to function properly.
These cookies help us understand how visitors interact with the website.
These cookies are used to deliver personalized advertisements.

